Topics
>RESEARCH
Innovative Therapies for Ischemic Stroke: Novel Bicarbonate-Sensing G Protein-coupled Receptor Shows Promise
Innovative Therapies for Ischemic Stroke: Novel Bicarbonate-Sensing G Protein-coupled Receptor Shows Promise
Researchers have identified this receptor in brain mural cells that regulates reperfusion injury.
Optimal pH homeostasis for cellular function is maintained by the acid-base balance through multiple buffering systems, such as the bicarbonate system, across the cell. Shifts in this equilibrium can impact health, prompting a closer look at how cells react under pathological conditions. While past studies have offered insights, several aspects remain unexplored. Researchers from Japan have now discovered a new bicarbonate-sensing receptor that regulates ischemic reperfusion injury and offers therapeutic insights into ischemic stroke treatment.
Cells actively rely on maintaining an appropriate acid-base balance to support optimal function. Under normal physiological settings, the pH inside cells remains within a controlled range. However, disruptions in this equilibrium have been linked to a wide range of health conditions, both minor and catastrophic. Changes in the extracellular environment are monitored by “membrane receptors,” of which the G protein-coupled receptors (GPCRs) are a large family of membrane proteins that mediate multiple cellular responses. However, the role of GPR30, also known as G protein-coupled estrogen receptor or membrane estrogen receptor, and its importance in cellular responses to acid-base disturbances have remained unclear.
In a groundbreaking study, a team of researchers from Juntendo University in Japan, led by Specially Appointed Associate Professor Airi Jo-Watanabe investigated the cellular responses to pH variations, with a particular focus on exploring the significance of GPR30. The study was recently published in Nature Communications on 27 February 2024, with Dr. Takehiko Yokomizo, Dr. Nobutaka Hattori, and Dr. Takahiro Osada as co-authors. This study marks a crucial step in our understanding of the mechanisms governing cellular behavior in response to changes in bicarbonate concentrations. Sharing insights from the research, Dr. Jo-Watanabe explains, “Our objective was to identify a GPCR associated with the acid-base balance, and while looking for targets, GPR30 grabbed our attention. We identified GPR30 as a bicarbonate-sensing GPCR and then shifted our focus to identifying its contribution to the pathophysiology of ischemic stroke.”
So, why did the researchers choose GPR30 for their study? While screening the Psychoactive Drug Screening Program (PDSP) database, the team came across 10 GPCRs that were predominantly expressed in the stomach and pancreas, of which four were highly expressed in the brain. As pathological conditions such as ischemia and reperfusion can disrupt the acid-base balance, affecting vascular and perivascular cells through receptors, the researchers looked for GPCRs highly expressed in brain microvasculature and identified Gpr30 as one of them. This fueled curiosity about GPR30’s role as a potential acid-base sensor in the brain. The team found that depleting bicarbonate from the culture medium lowered GPR30 activation (calcium responses) in GPR30-overexpressing MCF-7 and HEK cells, indicating that bicarbonate activates GPR30 in vitro.
The mouse myoblast C2C12 cell line was used to confirm that endogenous GPR30 is activated by bicarbonate ions in vitro. This was further validated ex vivo using GPR30 knock-in mice expressing the fluorescence reporter “Venus.” Confocal microscopy revealed strong expression of GPR30 in the brain microvasculature, particularly in pericytes, cells that help maintain homeostatic and hemostatic functions in the brain. This hinted at a potential mechanism for GPR30’s role in cerebrovascular regulation.
Next, they decided to study the role of GPR30 in cerebral ischemia-reperfusion injury (interruption and restoration of blood flow to tissues, causing cellular dysfunction), which is key to ischemic stroke pathophysiology. GPR30 deficiency was then explored in the context of ischemia-reperfusion injury, and the researchers observed GPR30-deficient mice exhibiting significant protection against this injury, showcasing reduced neurological deficits, blood-brain barrier disruption, and apoptotic cell death. Moreover, GPR30 deficiency led to improved blood flow recovery after ischemia-reperfusion injury, emphasizing its role in controlling blood flow in both large vessels and capillaries.
The bicarbonate buffer system supplies bicarbonate ions and protons to the acid/base sensing GPCR identified in this study, modulating signal transduction in tandem with the ever-changing extracellular environment. The unexpected connection between GPR30 and bicarbonate sensing invites further exploration into the mechanisms governing cerebrovascular health, offering a potential avenue for targeted strategies to alleviate the impact of ischemic stroke reperfusion injury. Dr. Jo-Watanabe concludes by saying, “Our findings pave the way for a revolutionary approach to modulating vascular reactivity to support overall health by fine-tuning homeostatic vasoreactivity via the bicarbonate receptor.”
In conclusion, this research could mark a paradigm shift in our understanding of receptor roles in cerebrovascular regulation.
***
Regulation of ischemia-reperfusion injury through a bicarbonate-sensitive G protein-coupled receptor.
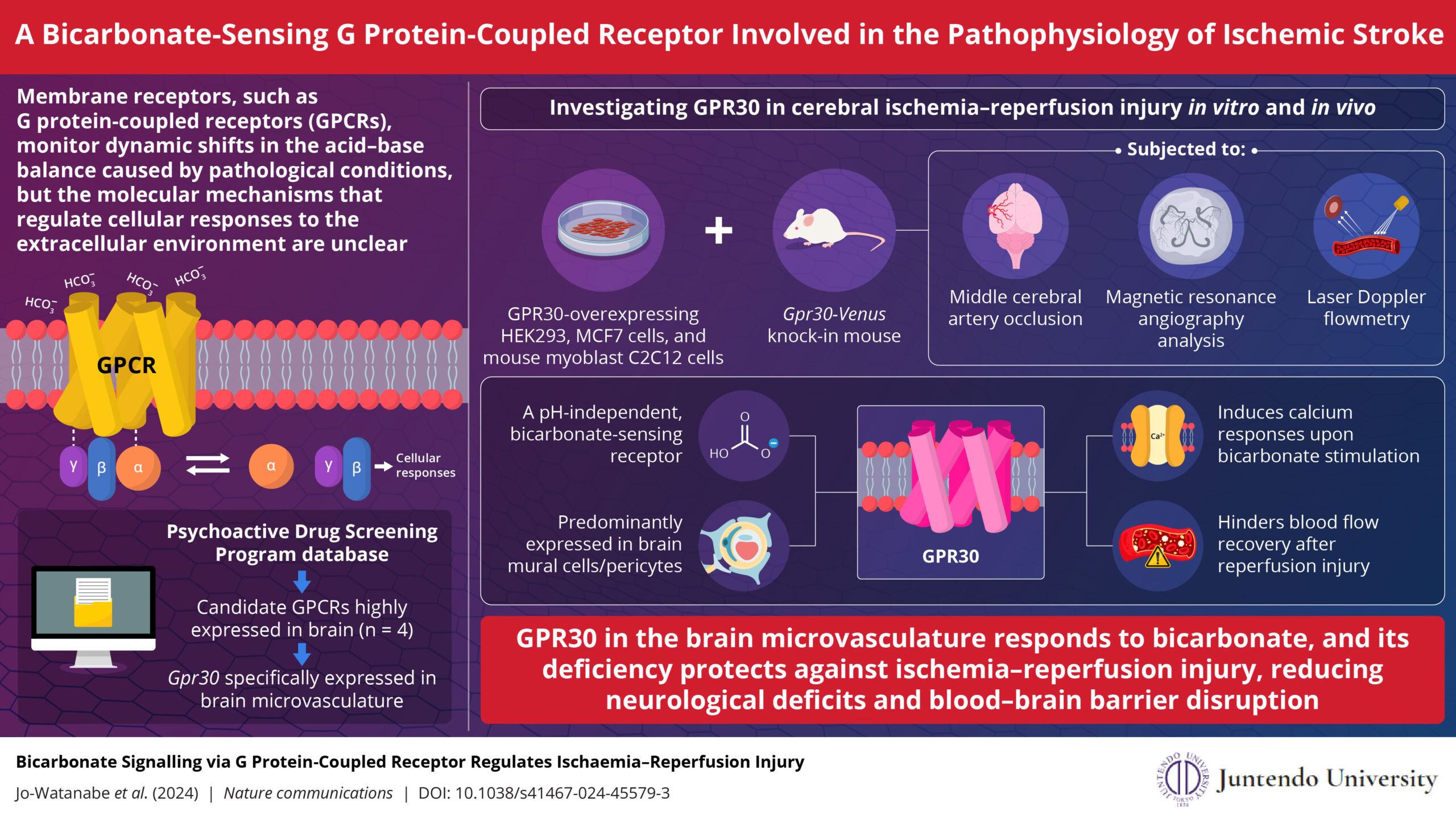
Image caption: GPR30 in brain microvasculature responds to bicarbonate, and its deficiency protects against ischemia-reperfusion injury, reducing neurological deficits and blood-brain barrier disruption. These findings offer insights into developing innovative clinical approaches for ischemic stroke.
Image credit: Dr. Airi Jo-Watanabe of Juntendo University Graduate School of Medicine
License type: Original content
Usage restrictions: You are free to share and adapt the Infographic material but attribution is required, with a link to the news source.
***
About Dr. Airi Jo-Watanabe
Dr. Airi Jo-Watanabe is a specially appointed Associate Professor at the Department of Biochemistry, Juntendo University Graduate School of Medicine. She has 13 English and 10 Japanese publications to her name in the field of medical biochemistry and nephrology. Her specific areas of interest include G-protein-coupled receptors, intracellular signaling, vascular biology, and nephrology. She is a member of several recognized societies like the Japanese Biochemical Society, the Japanese Society of Nephrology, and the Japanese Society of Internal Medicine.
***
Reference
|
Authors |
Airi Jo-Watanabe1,2, Toshiki Inaba3, Takahiro Osada4, Ryota Hashimoto5, Tomohiro Nishizawa6, Toshiaki Okuno1, Sayoko Ihara7, Kazushige Touhara7, Nobutaka Hattori3,8, Masatsugu Oh-Hora1,5, Osamu Nureki9, and Takehiko Yokomizo1 |
|
Title of original paper |
Bicarbonate signalling via G protein-coupled receptor regulates ischaemia reperfusion injury |
|
Journal |
Nature Communications |
|
DOI |
|
|
Affiliations |
1Department of Biochemistry, Juntendo University Graduate School of Medicine 2AMED-PRIME, Japan Agency for Medical Research and Development 3Department of Neurology, Juntendo University School of Medicine 4Department of Neurophysiology, Juntendo University School of Medicine 5Laboratory of Cell Biology, Biomedical Research Core Facilities, Juntendo University Graduate School of Medicine 6Graduate School of Medical Life Science, Yokohama City University 7Department of Applied Biological Chemistry, Graduate School of Agricultural and Life Sciences, The University of Tokyo 8Neurodegenerative Disorders Collaborative Laboratory, RIKEN Center for Brain Science 9Department of Biological Sciences, Graduate School of Science, The University of Tokyo |